1. 孤立的avL导联出现Q波(反映侧壁向量的其他导联无异常Q波及ST-T改变)时,嘱患者深吸气后深呼气再屏气描记心电图,若Q波减小或消失,为正常变异。
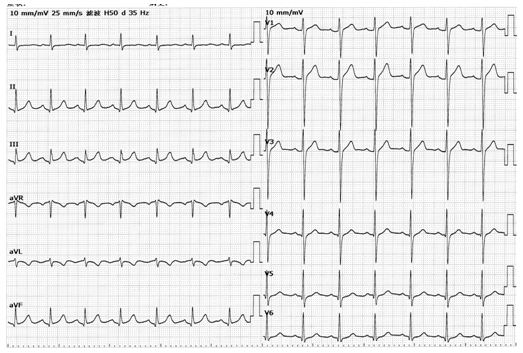
2. 正常情况下,avR导联可出现Q波或QS波。(见图6)
3. ⑴孤立的Ⅲ导联出现Q波时,嘱患者深吸气后屏气描记心电图,若Q波减小或消失,为正常变异;
⑵Ⅲ、avF导联出现Q波伴Ⅱ导联有q波或出现ST段抬高和/或T波倒置时考虑下壁心肌梗死;
⑶Ⅲ、avF导联出现Q波伴右胸导联ST段压低或T波高耸或V1导联的R/S≥1时考虑下壁心肌梗死。
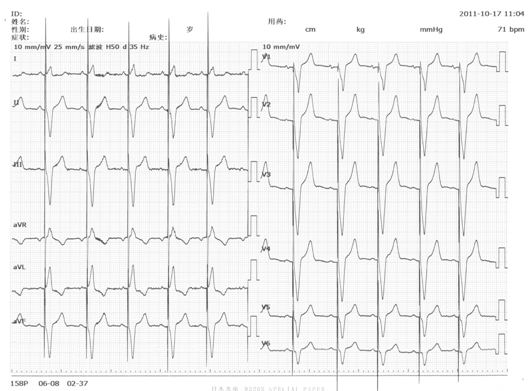
4. V1、V2导联不可有q波,但偶可呈QS型,V3导联很少有q波。而后再与下列情况相鉴别。
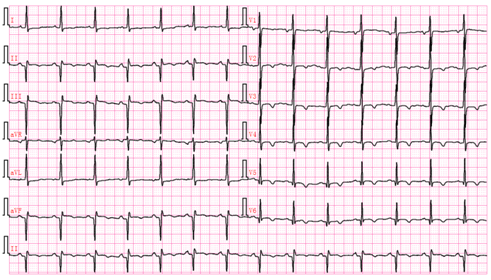
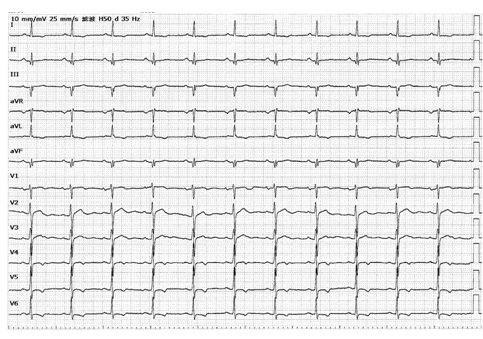
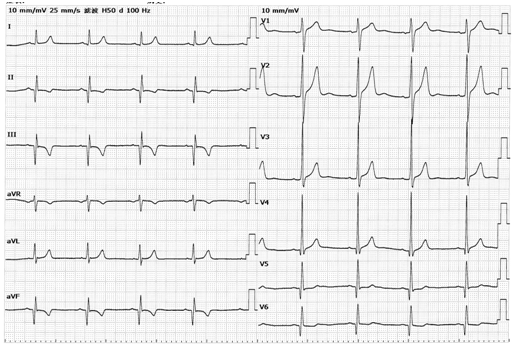
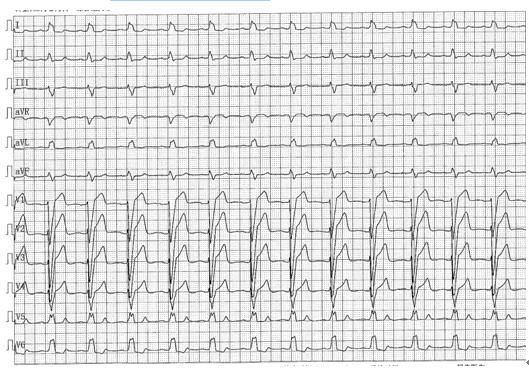
图5-2 A胸导联电极位置错放描记心电图
(V1、V2导联位置错放)
等位性Q波(isopotential Q wave):
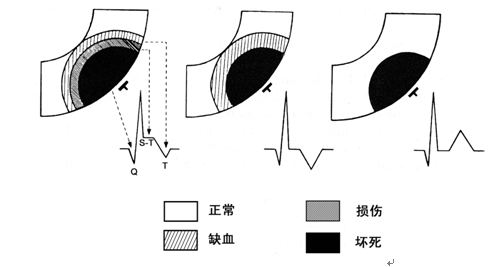
发生心肌梗死时,由于梗死面积、厚度、部位等因素未形成典型的病理性Q波,而产生各种特征性QRS波群形态改变(见图7)。其具有以下特点:
(1)q波时限≥0.03 s,但其振幅<0.1 mv,同时伴有切迹或粗顿。
(2)Ⅲ导联为病理性Q波,avF导联q波仅时限≥0.03 s,Ⅱ导联q波形态、时限、振幅均正常;此时avR导联有r波则支持陈旧性下壁心肌梗死。
(3)V1、V2导联呈qrS型,应排除右心室肥厚(右心室肥厚应伴有电轴右偏,且V3R、V4R呈qR型)。
(4)新出现的小Q波递增不良,即qV3>qV4,qV4>qV5,qV5>qV6。
(5)Q波区:梗死区导联周围均可记录到q波,当某个胸导联q波未达病理性Q波诊断标准而又怀疑心肌梗死时,需加做上、下肋间导联或将电极左右轻度偏移描记心电图。
(6)进展性Q波:同一患者在相同体位条件下(胸导联电极安放位置应做标记,每次固定同一位置描记)24小时内多次检查心电图进行动态观察,原有Q波的导联出现Q波进行性增宽、加深;或无Q波的导联出现新的q波,并能排除间歇性室内阻滞或心室预激。
(7)间隔性Q波丢失:即Ⅰ、avL、V5、V6导联q波消失或减小。
(8)QRS波群改变:V4~V6导联QRS波群R波起始有切迹、顿挫,出现>0.5mv的负向波,提示小面积心肌梗死。
-
V1~V4导联R波递增不良或R波反向递增,即RV1>RV2、RV2>RV3、RV3>RV4、RV4>RV5。(见图8)
-
相邻两个导联的R波振幅相差>50%,如RV3>1/2RV4。
-
同一导联的R波振幅在不同次心电图记录中呈进行性降低或消失。
-
V1、V2导联R波增大时可能为正后壁心肌梗死的镜像观,需常规加做V7~V9导联。(见图9)
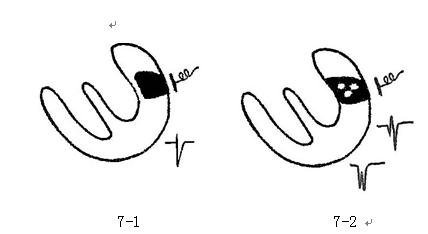
图7 等位性Q波形成示意图
7-1图显示顿抑存活心肌电功能恢复,面对电极的向量形成r波
7-2图显示顿抑存活心肌与坏死心肌相对位置不同而形成多种形态QRS波
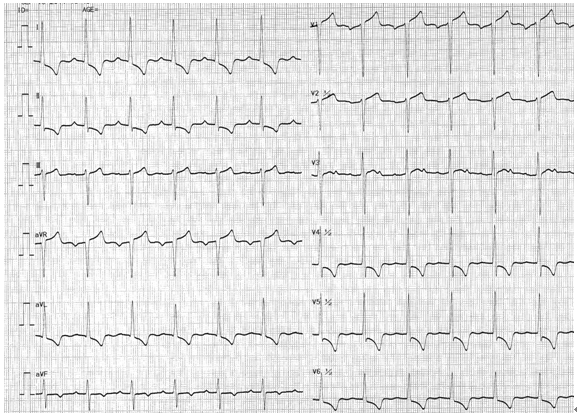
图9 陈旧性下壁心肌梗死伴V1导联R波高
及V5、V6导联梗死性Q波
(9)RⅢ、RavF<0.25mv伴QⅡ存在;或RⅡ<0.25mv伴QⅢ、QavF存在。
(二)非梗死性Q波:指心肌梗死以外的病症所引起的异常Q波。多发生于Ⅰ、avL、Ⅱ、Ⅲ、avF、V1~V3导联。
5.1 肥胖、妊娠或其他原因造成的膈肌上抬,会使心电轴左偏在下壁导联产生非梗死性Q波。
(1)当心室除极初始向量额面指向00~+300,Ⅲ导联出现Q波,而Ⅱ、avF导联不出现Q波。
(2)当心室除极初始向量额面指向00~-300时,Ⅲ、avF导联出现Q波,Ⅱ导联不出现Q波。
(3)当心室除极初始向量额面指向-300以上时,Ⅱ、Ⅲ、avF导联均出现Q波。
嘱患者深吸气(膈肌下降)后屏气描记心电图,可使上述情况的Q波减小或消失。
(1)左心室肥大:可出现指向左后方的起始向量,抵消了正常指向右前方的室间隔除极向量,使V1、V2导联起始r波减小或消失而出现QS波,描记该两个导联低一肋间心电图会显示rS型。(见图10)
(2)右心室肥大:心脏会出现顺钟向转位,室间隔除极方向变为由右向左,造成Ⅰ、avL导联出现QS波;右胸导联出现高R波,需与正后壁心肌梗死相鉴别,但V1导联T波在右心室肥大时倒置、在正后壁心肌梗死时高耸。(见图11)
(1)心绞痛:心绞痛发作时,某支冠状动脉因狭窄或痉挛使该区产生严重缺血而丧失了电活动,使心室除极向量背离电静止区出现Q波;但当缺血心肌恢复了血供,心肌的电动力随之恢复,Q波消失;故又称为急性可逆性心肌梗死。
(2)急性重症心肌炎:心肌不同程度的损伤、坏死,可出现非梗死性Q波,但缺乏心肌梗死ST-T特征性演变规律。
A、肥厚型心肌病时由于室间隔增厚引起自左向右的心室初始除极向量增大,且其激动顺序发生改变。致Ⅰ、Ⅱ、avL、avF、V5、V6导联出现异常Q波,但该Q波窄而深,T波直立,形态高尖。(见图12)
B、扩张型心肌病会使左室某部位心肌电活动丧失产生非梗死性Q波。心电图V1~V4导联出现非梗死性Q波,有时呈QS型,或胸导联R波递增不良,注意与陈旧性前间壁心肌梗死相鉴别。
继发性心肌病时心肌变性及纤维化、瘢痕形成使心肌电活动显著减退或消失产生非梗死性Q波。
5.5 肿瘤转移累及心肌:偶见非梗死性Q波,可伴P波异常、QRS波群低电压、ST段改变。
(1) 左束支阻滞:可使室间隔除极异常及左心室延缓除极造成V1~V3导联起始r波变小或出现QS波伴ST段抬高。(见图13)
(2)左前分支阻滞:除极初始向量指向左后下方,可使Ⅰ、avL导联出现q波或原q波增大。(见图14)
图14 完全性右束支阻滞、左前分支阻滞
伴陈旧性前间壁心肌梗死
(3)右束支阻滞:某些患者V1、V2导联在发生右束支阻滞前呈QS型,合并右束支时则呈qR型,易与前间壁心肌梗死相混淆,但此qR型不会出现在V3导联。(见图15)
5.7 心室预激:房室之间存在异常传导束使心室提前激动;由于房室旁路位置不同,初始除极方向发生改变,使某些导联出现非梗死性Q波。心电图具有PR间期缩短、预激波及QRS波增宽的特征性改变。
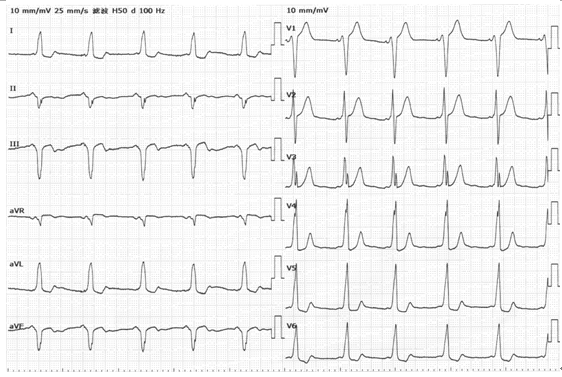
(1)A型心室预激:房室旁路的心室端可能止于左心室的后底部,初始向量指向前方,在右胸导联出现高宽的R波,类似正后壁心肌梗死。旁道靠后在Ⅱ、Ⅲ、avF导联出现非梗死性Q波,类似下壁心肌梗死、后壁心肌梗死图形。(见图16)
图16
患者男,34岁,体检发现心电图显示PR间期缩短伴QRS波起始预激波,V1~V6导联QRS波主波及预激波方向向上,Ⅲ、avF导联呈QS型
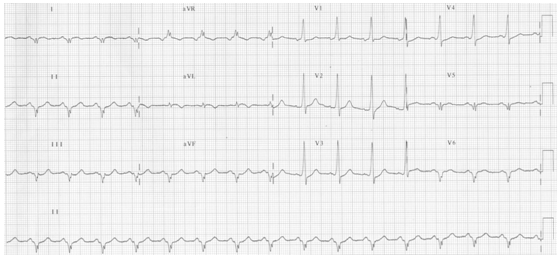
(2)B型心室预激:房室旁路心室端可能止于右心室的前壁或侧壁,初始向量指向左、后,致下壁或右胸导联出现QS波,类似下壁或前间壁心肌梗死。(见图17)
图17
患者女,43岁,心电图显示PR间期缩短伴QRS波起始预激波,V1导联QRS波主波及预激波方向向下,Ⅱ、Ⅲ、avF导联有非梗死性Q波
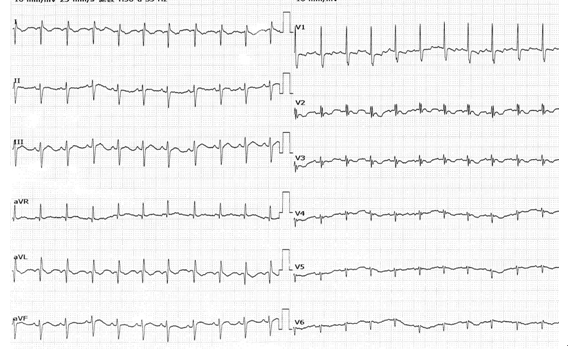
(3)C型心室预激:房室旁路心室端可能止于左心室前壁侧壁,初始除极指向右前,Ⅰ、V5、V6有时并Ⅱ、Ⅲ、avF导联出现非梗死性Q波,类似下壁、前侧壁心肌梗死。(见图18)
图18
患者男,46岁,因酒后心慌、胸闷就诊,心电图显示PR间期缩短伴QRS波起始预激波,V1~V4导联QRS波主波及预激波方向向上,而Ⅰ、avL、Ⅱ、Ⅲ、avF、V5、V6导联均有非梗死性Q波
(1)肺气肿:伴右心室肥大时心脏顺钟向转位,可致Ⅱ、Ⅲ、avF导联及右胸导联出现QS波。
(2)肺栓塞:Ⅰ导联出现S波并增宽,Ⅲ导联Q波加深伴T波倒置。
(3)肺心病:心脏顺钟向转位,V1~V4导联呈QS型,伴SⅠSⅡSⅢ征。
5.9 左侧气胸:范围较大时可致心电轴右偏、QRS波群低电压、胸导联R波振幅降低或呈QS型。
5.10 脑血管疾病:急性脑血管病后一至数日,脑交感神经中枢直接或间接受到刺激,释放过多的儿茶酚胺;心电图中部分或多数导联R波振幅降低、甚至出现非梗死性Q波。
5.11 急性胰腺炎:患者剧烈疼痛伴交感神经兴奋性增高,反射性地使冠状动脉收缩,加重心肌缺血致心肌顿抑;或因局部电解质紊乱使心肌细胞膜电位改变致除极异常形成非梗死性Q波。
5.12 完全性校正型大血管转位:左右心室反位,室间隔除极初始向量由右向左,致右胸导联呈QS型伴其他一个或多个导联出现非梗死性Q波。
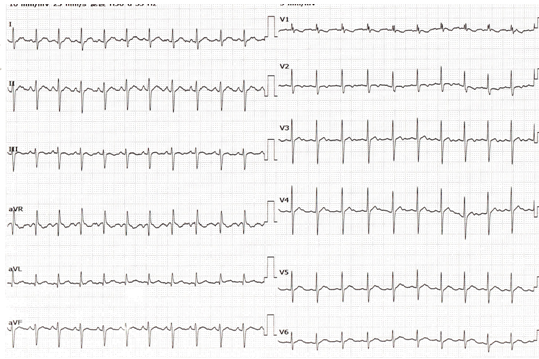
5.13 右位心:是心脏在胸腔的位置移至右侧的总称。Ⅰ、avL导联出现非梗死性Q波,伴胸导联R波振幅递减。(见图19)
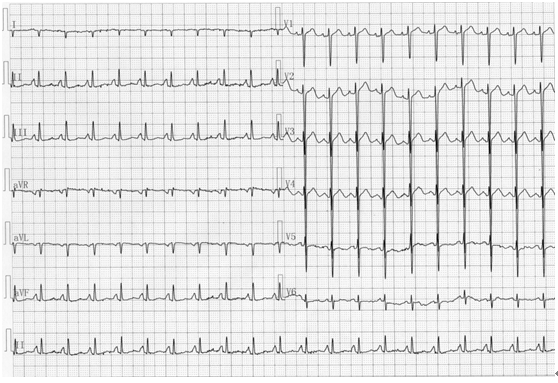
图19-1
患者男,48岁,因急性胰腺炎就诊,心电图示右位心(左右手正常连接)
5.14 右旋心:即假性右位心,此时心脏大部分位于右胸腔,而心尖朝向右前方,但各心腔间左右关系保持大致正常。Ⅰ、avL或Ⅱ、Ⅲ、avF导联出现非梗死性Q波。
5.15 先天性左侧心包缺如:胸导联R波递增不良,V1~V3导联可呈QS型,V4导联r波小。
5.16 人工心脏起搏器植入术后:心室电极置于右心室心尖部时,Ⅱ、Ⅲ、avF和V1~V4导联的心室起搏图形多呈QS型。(见图20)
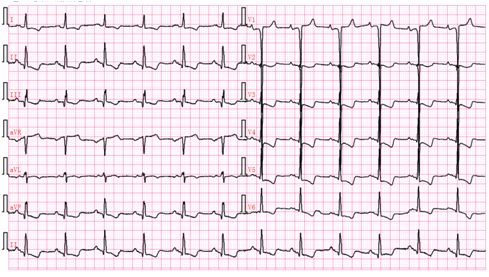
图20
女,73岁,植入双腔起搏器一年后随访心电图